What is the prostate?
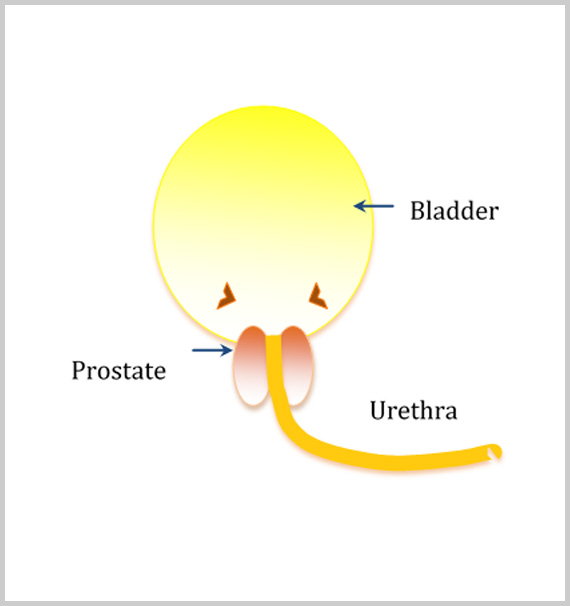
The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows from the bladder and out through the penis. The prostate gland contributes to the seminal fluid produced during ejaculation.
Prostate cancer
Prostate cancer is the most common cancer in Australia men effecting around 20,000 men each year. It is the third most common cause of cancer death, with >3,000 men dying in Australian from prostate cancer each year. The most common age of diagnosis is between 60-65yo. The majority (>99%) of prostate cancers are adenocarcinoma.
Symptoms and signs of prostate cancer
Due to PSA testing, most men diagnosed with prostate cancer will have no symptoms however symptoms that can occur with presentation include:
- Blood in the urine (Haematuria) – the present on blood in the urine, which can be either visible (frank or macroscopic haematuria) or on dip-stick or laboratory testing (microscopic haematuria) should also be investigated further.
- Voiding difficulty – this can include hesitancy (difficulty starting urination), slow stream, intermittency (urine stops and starts), urgency (the sudden need to pass urine), frequency (passing urine often) and leaking urine (incontinence).
- Bone pain – persistent pain in the back, hip or ribs which is difficult to control.
- Weight loss and fatigue
- Declining renal function
Risk factors
The main risk factor for prostate cancer is being a male over 55yo.
Only a small percent of cancers are due to inherited conditions. The most common inherited genes associated with prostate cancer are BRAC1 and BRAC2. BRAC1 and 2 are associated with increased risk of breast and ovarian cancer in women. These genes produce tumour suppressor proteins that help repair damaged DNA. If these genes are faulty the proteins are either not produced or are defective, meaning DNA damage may not be repaired properly. As a result, cells are more likely to develop additional genetic alterations that can lead to cancer.
There is an association between a diet high in animal fat and low in fruit and vegetables and a high risk of prostate cancer. Also men of African descent are at higher risk.
Diagnosis
To diagnosis prostate cancer, a pathologist needs to see evidence of cancerous changes in a tissue specimen. This means a biopsy is required to make the diagnosis.
The first step to diagnoses therefore is to identify which men need a biopsy. A PSA blood test is the most common test that can help identify which men are at high enough risk of harbouring prostate cancer to warrant a biopsy. A PSA above the 95th percentile, that is a PSA in the top 5%, is associated with a 30% risk of prostate cancer. That is, 1 in 3 men with an elevated PSA will have cancer in their prostate.
A properly conducted MRI can help identify where in the prostate, a cancer may be. This can help target a biopsy better however MRI will miss up to 15% of cancers therefore it often does not allow you to forgo a biopsy.
Treatment
The management of prostate cancer is dependent on cancer factors and patient factor.
Cancer Factors
Cancer factors are the grade and stage of the cancer.
Grading
Grading answers the question: How aggressive (or fast growing) is my cancer.
Prostate cancer is frequently described in three categories, low, intermediate and high risk cancer. This risk is mostly dependent on cancer grade but other factors like PSA can influence this. Until recently prostate cancer grade was described using the Gleason grading system however this recently changes to the ISUP/ WHO grade group.
| ISUP/WHO* Grade Group | Gleason score | Histological features |
| 1 | 3+3=6 | Only individual discrete well formed glands |
| 2 | 3+4=7 | Predominately well-formed glands with small component of poorly formed glands |
| 3 | 4+3=7 | Predominately poorly formed glands |
| 4 | 8 | Only poorly formed glands |
| 5 | 9-10 | Lack of gland formation |
*(International society of urological pathology/ World health organisation).
Staging
Staging answers the question: Where is the cancer? Has it spread?
Prostate cancer starts in the prostate. It can spread locally or distantly. The spread is described using a common cancer classification system called TNM: T (tumour), N (Lymph nodes); M (Metastasis).
Prostate cancer TNM classification
| TNM | Classification | Features |
| T | 1 | Tumour confined to the prostate and non-palpable |
| 2 | Tumour confined to the prostate but palpable | |
| 3 | Tumour extending through the prostate capsule +/- into seminal vesicles | |
| 4 | Tumour extending into adjacent structures (Bladder, rectum etc) | |
| N | 1 | Local regional lymph nodes involved |
| M | 1 | Distant lymph nodes, bone or other organs involved |
Identifying the location of prostate cancer is dependent on imaging tests (CT, bone scan, PET (PSMA) scan and MRI). These tests are best at detecting macroscopic deposits of disease so even if the tests are negative there is still a risk microscopic areas of cancer may be present. This is why even after treatment you need monitoring.
Patient Factors
There are many ways to treat prostate cancer. Prostate cancer treatment therefore needs to be individualised for each man. This means the best treatment option for can man has taken into account not only the stage of the cancer but also their overall health, prior surgical procedures, current medical conditions and medications. It also requires assessing their personal preferences and lifestyle needs.
Treatment options
Treatment options for prostate cancer include surveillance, surgery, radiotherapy and pharmaceutical. There are different indications for all three:
| Treatment option | Suitable cancers | Involves |
| Active Surveillance | Low grade, low volume cancer | Accepts the factor that most men with this cancer will not experience symptoms or complications from the cancer in their lifetime. These men are closely observed, with regular reviews including blood tests and repeat prostate biopsy. If there is evidence that the cancer is progressing, treatment will be offered at a time when cure is still possible. |
| Radical prostatectomy |
Intermittent/ High risk Organ confined |
When cancer is confined to the prostate gland. Involves surgical removal of the entire prostate gland and seminal vesicles. Has the potential to cure a man of cancer. |
| Radiotherapy |
Intermittent/ High risk Organ confined |
When cancer is confined to the prostate gland. Involves surgical removal of the entire prostate gland and seminal vesicles. Has the potential to cure a man of cancer. |
|
ADT (Androgen deprivation therapy) |
Metastatic disease | Prostate cancer growth is dependent on testosterone. Decreasing testosterone production, which medication, results in halting cancer growth. This treatment is typically offered when the cancer has spread (metastasized) outside the prostate. |
| Chemotherapy and Targeted therapy | Castrate resistant Metastatic disease | Castrate resistance occurs when the cancer is able to keep growing despite the testosterone levels being low. |
| Watchful waiting | Prostate cancer | Accepts that the man will not experience symptoms or complications from the cancer in their lifetime. He is observed at regular intervals. If symptoms start to occur or evidence suggests symptoms will occur in the near future, treatment is started. Treatment is aimed only at slowing down the cancer not curing the cancer. |
*(International society of urological pathology/ World health organisation).
KEY POINTS
- Prostate cancer is the most common cancer in men (>20,000 men diagnosed each year).
- Prostate cancer is the third most common cancer death (>3,000 men dying each year).
- Prostate cancer can be cured if diagnosed when confined to the prostate.
- When prostate cancer is confined to the prostate the only sign of its presence may be an elevated PSA.
- Prostate cancer requires a biopsy for diagnosis
- Quality of life and life expectancy can be improved with treatment of prostate cancer
- Prostate surgery can be done key-hole (robotics) to minimise recovery time.
- Not all men with prostate cancer need immediate treatment instead active surveillance is appropriate.
